Introduction
Idiopathic scrotal calcinosis is a rare, benign dermatological condition first described by Lewinski in 1883 [1]. It is characterized by the presence of multiple calcified nodules within the scrotal skin, typically affecting men in their second to fourth decades of life. The exact etiology remains unclear, though theories suggest dystrophic calcification of preexisting epidermoid cysts, eccrine duct milia, or degeneration of dartos muscle. Idiopathic scrotal calcinosis is often asymptomatic, but lesions may cause cosmetic concern or pruritus [2]. We present a case of Idiopathic scrotal calcinosis in a young Ghanaian male, including clinical presentation, diagnostic workup, surgical management and histopathological confirmation.
Case presentation
A 34-year-old male presented to the outpatient department with a ten-year history of increasing nodular lesions on the left scrotum. The nodules gradually increased in number and size over the years. He reported no associated pain but complained of itching, especially during walking or physical activity. He denied trauma, infections, prior surgery or systemic illness.
On examination, multiple firm, non-tender nodules were observed on the left scrotal skin. The smallest lesion measured approximately 2 mm in diameter and the largest about 7 mm in diameter (Figure 1). All nodules were fixed to the overlying skin but not attached to the underlying testicular structures. There were no signs of inflammation, discharge or inguinal lymphadenopathy.
Initial evaluation included a dermatology consultation, after which the patient was referred to the urology unit for surgical consideration. Scrotal ultrasonography showed multiple wellcircumscribed hyperechoic nodules within the scrotal skin layers without involvement of deeper tissues or testicles, suggestive of scrotal calcinosis.
Routine laboratory investigations, including a full blood count, serum urea, creatinine, and electrolytes, as well as serum phosphate, calcium and parathyroid hormones, were within normal limits. Chest X-ray and transthoracic echocardiography were also unremarkable.
The patient was booked for elective excision under spinal anaesthesia. Intraoperatively, multiple calcified nodules were excised from the scrotal skin without breaching the tunica vaginalis or involving the testicular parenchyma. The skin was sutured with good cosmetic closure.
Histopathological findings confirmed the diagnosis: sections of the excised scrotal skin revealed dermal nodules consisting of fibrous tissue and amorphous basophilic calcium deposits, with no epithelial lining, consistent with idiopathic scrotal calcinosis.
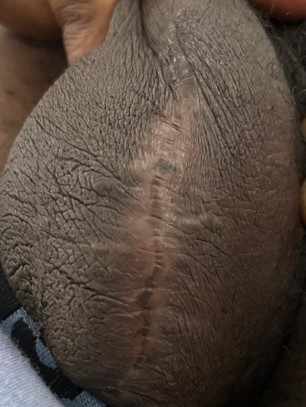
Postoperative recovery was uneventful. At two-week, sixweek and 6-month follow-ups, the patient had healed well with no recurrence or new nodules and was satisfied with the cosmetic outcome (Figure 2).
Discussion
Idiopathic scrotal calcinosis, though benign, presents diagnostic and therapeutic challenges due to its rare nature and unclear etiology. Several theories exist: the most accepted being dystrophic calcification of sebaceous or epidermoid cysts. However, in many cases, including this one, histology fails to identify epithelial remnants, suggesting a truly idiopathic nature [3].
The absence of systemic metabolic abnormalities (e.g., normal calcium, phosphate, and parathyroid hormone levels) in this case further supports the idiopathic diagnosis. Imaging modalities such as ultrasound play a crucial role in delineating lesion depth and excluding involvement of testicular structures [4].
Surgical excision remains the primary treatment option. Complete excision of all nodules with primary skin closure yields excellent outcomes and minimal recurrence risk. The choice of spinal anesthesia in this case provided adequate analgesia and improved postoperative comfort [3].
Histopathology remains the gold standard for diagnosis. The findings in this case – calcium deposits without epithelial lining – are consistent with literature descriptions of idiopathic calcinosis [5].
Conclusion
Idiopathic scrotal calcinosis is a rare, benign condition that should be considered in patients with long-standing, painless scrotal nodules. Diagnostic evaluation involves ruling out metabolic abnormalities and confirming the diagnosis via histopathology. Surgical excision offers definitive treatment with excellent cosmetic results. Early recognition and appropriate referral are essential for effective management.
Declarations
Author contributions: Dennis Awedam Achio: Conceptualization; formal analysis; investigation; methodology; writing – original draft; writing – review and editing. Eunice Wilberforce A. Achio: Review and editing. Derick Boateng: Review and editing.
Acknowledgement: The authors extend profound gratitude to the nursing staff of the urology ward at the University of Ghana Medical Center for their hard work and care for all patients.
Funding information: The authors did not receive funding for the publication of this article.
Conflict of interest: There are no conflicts of interest.
Data availability statement: Data sharing is not applicable
Ethical statement: Ethical approval was not applicable. The study was conducted in accordance with the Declaration of Helsinki.
Consent: The authors certify that written informed consent was obtained from the patient to publish this report.
References
- Tareen A, Ibrahim RM. Idiopathic scrotal calcinosis A case report. Int J Surg Case Rep. 2018; 44: 51-53.
- Khallouk A, Yazami OE, Mellas S, Tazi MF, El Fassi J, Farih MH. Idiopathic scrotal calcinosis: a non-elucidated pathogenesis and its surgical treatment. Rev Urol. 2011; 13: 95-97.
- Kyei MY, Djagbletey R, Abrahams AD, Mensah JE. Idiopathic scrotal calcinosis: A case report and review of postoperative outcomes. Case Rep Urol. 2020; 2020: 8877695.
- Wright S, Navsaria H, Leigh IM. Idiopathic scrotal calcinosis is idiopathic. J Am Acad Dermatol. 1991; 24: 727-730.
- Peters MS, Winkelmann RK, Wolff K. Calcinosis cutis: a study of 51 cases. Arch Dermatol. 2003; 139: 1069-1077.
- How to cite this article: Achio Awedam D, et al. Idiopathic scrotal calcinosis: A Case Report and surgical outcome.