Introduction
Myasthenia gravis is chronic autoimmune incurable disease whose cause is not well known. The antibodies produced affect the neuromuscular junction and cause variable fatigability of skeletal muscles [1,2]. It is divided into 4 types: (Ocular, bulbar, respiratory and musculoskeletal). MG crisis may be precipitated by many factors: Surgery, physical stressors, emotional stress, pain, temperature extremes, sleep deprivation, premenstrual state, pregnancy, drugs and immune modulation [3].
Thymoma operations are the ones which are commonly associated with MG crisis [4].
Case presentation
A 41-year-old male accountant presented with a history of abdominal pain, on and off constipation alternating with diarrhoea for the last 5 years. But with no history of nausea, vomiting, abdominal distension, rectal bleeding or hemorrhoids. Over the previous 3 months he had lost appetite. He had been treated in different health units with dietary regulations and assorted laxatives with no improvement. The reason for referral to us was recurrent abdominal pain.
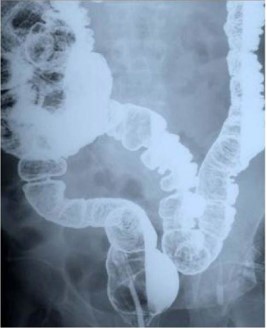
Physical evaluation revealed a middle-aged man who looked healthy, not anaemic and no lymphadenopathy. Abdominal and per rectal examination revealed no abnormal findings and central nervous examination was normal. A barium meal Figure 1 revealed a symptomatic redundant sigmoid colon. A diagnosis of ‘symptomatic redundant sigmoid colon’ grade III [5] was made.
He was counselled and consented to an open sigmoidectomy and primary end to end anastomosis.
Preoperatively the heamoglobin content was 14 g/dl, fasting blood glucose of 6 mMol/L, he was blood group O+ and seronegative for HIV. Other preparations included low fibre diet for 5 days, a warm soap enema in the morning before surgery, nil per os starting at 10.00 pm the previous evening and review by the anaesthesiology team.
The operation lasted 1 hour and 30 minutes and was uneventful.
Post operatively, after a short stay in the recovery room, he was transferred to the parent ward. The following were prescribed: IV fluids of N. saline and 5% dextrose in a ratio of 1: 3 totaling to 3l in 24 hours running at 33 drops per minute. IV paracetamol 1 g every 6 hours for 2 days, IM gentamycin 160 mg od for 3 days and IV metronidazole 500 mg 8 hourly for 3 days. He did not have a nasogastric tube or flatus tube.
The operation ended at 11.00 AM.
At 3.00 PM on the same day he developed musculoskeletal symptoms of MG crisis. He did not have ocular, bulbar or respiratory symptoms.
A neostigmine test was done [6] and the response was positive. He was treated on the ward with pyridostigmine 60 mg 8 hourly [7] and improved.
After 3 days he was discharged and he returned after 6 days for removal of stitches. He had no side effects of pyridostigmine (diarrhea, vomiting, cold sweats, blood vision or tearing eyes).
Further investigations for MG were carried out [8]. The CTS of the chest showed no enlarged thymus reminant, other tests were within normal limits (Vit.B12 was 279 pmol/L, TSH was 4.0 pmol, Free T4 was 1 ng/dl, Total T3 was 110 ng/dl, Ach-R was <0.11 nmol/L. MUSK repetitive nerve test and single fiber electromyogram were not done. Histology showed no myenteric ganglia hyperplasia or aganglioneurosis of the sigmoid colon.
After 6 months he was wined off the pyridostigmine but the symptoms recurred. He was put back on pyridostigmine and after 2 years he was well. He was being followed up (The use of other drugs like steroids, immunosupressants and chemotherapy were not considered yet).
Discussion
Symptomatic redundant sigmoid colon is an entity where the sigmoid colon lengthens, dialates, causes abdominal pain, constipation alternating with diarrhoea and may twist and untwist on its narrow mesentery and cause symptoms which may resolve after taking some laxatives. Among some people at one point in time it twists and remains twisted and presents as a sigmoid volvulus in the emergency department as an abdominal emergency. The sigmoid volvulus in Uganda is common among male above 40 years of age. The symptomatic redundant sigmoid colon precedes a sigmoid volvulus and it has IV stages (During stage III the recommended treatment is sigmoid colectomy and primary end to end anastomosis in one layer. Usually, the operation is uneventful. The risks which make patients with symptomatic redundant sigmoid colon progress to sigmoid volvulus are not known. Some individuals live with a redundant sigmoid colon all their life time which is asymptomatic.
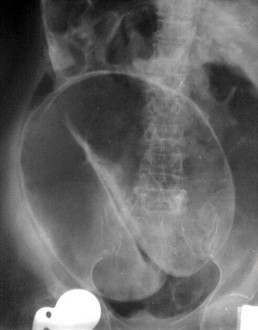
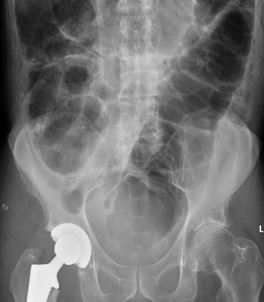
When the redundant sigmoid colon becomes symptomatic, the differential diagnosis is ‘acute colonic pseudo-obstruction’ which is associated with ‘intestinal neural dysplasia’ [9]. The erect plain abdominal x-ray appears different from that of a sigmoid volvulus (Figures 2 & 3).
During the literature review we did not find any publication reporting MG crisis following sigmoidectomy for a symptomatic redundant sigmoid colon which we are reporting in this paper for the first time.
Conclusion
Post operatively MG crisis may be precipitated by sigmoidectomy in adults.
Recommendation: It is recommended that post operatively after colectomy, symptoms of MG crisis should be looked for.
If MG crisis is suspected it can be confirmed by a neostigmine test and may be treated with pyridostigimine. Later other tests should be carried out. If the MG crisis is severe and affects the respiratory system the patient must be transferred to ICU for further treatment.
Patients satisfaction: The patient was satisfied with the treatment.
Consent: A written informed consent was obtained from the patient before publication of this report and images.
References
- Herr KJ, Shen SP, Liu Y, et al. The growing burden of generalized myasthenia gravis: a population-based retrospective cohort study in Taiwan. Front Neurol. 2023; 14: 1203679.
- Jie Ying Tan, Cheng Yin Tan, Prasana Nair Gengadharan, et al. Clinical characteristics and outcomes of myasthenia gravis in Malasia: A single-center experience. J Clin Neurol. 2024; 20: 412-421.
- Nacu A, Andersen JB, Lisnic V, et al. Complicating autoimmune diseases in myasthenia gravis: A review.
- Autoimmunity. 2015; 48: 362–368.
- Sussman J, Farrugia ME. Maddison P. Myasthenia gravis: association of British Neurologists’ management guidelines. Pract Neurol. 2015; 15: 199-206.
- Gakwaya AM. Sigmoid volvulus: WWW.gakwayamedicalnotes. com 2015.
- Rossen T, Rousseff: Diagnosis of Myasthenia gravis. Semin Neurol. 2015; 35: 327–339.
- Remijn-Nelissen L, Verschuuren JJ, Tannemaat MR. The effectiveness and side effects of pyridostigmine in the treatment of myasthenia gravis: a cross-sectional study. Neuromuscul Disord. 2022; 32: 790–799.
- Punga AR, Maddison P, Heckmann JM, Guptill JT, Evoli A. Diagnostics, and biomarkers of autoimmune neuromuscular junction disorders. Front Neurol. 2023; 14: 1203679.
- Daoud Magda MD, Haddad Fady G, MD Morcus, et al. Acute colonic pseudo-obstruction. American Journal of Gastroenterology. 2016; 1110: S603-S604.